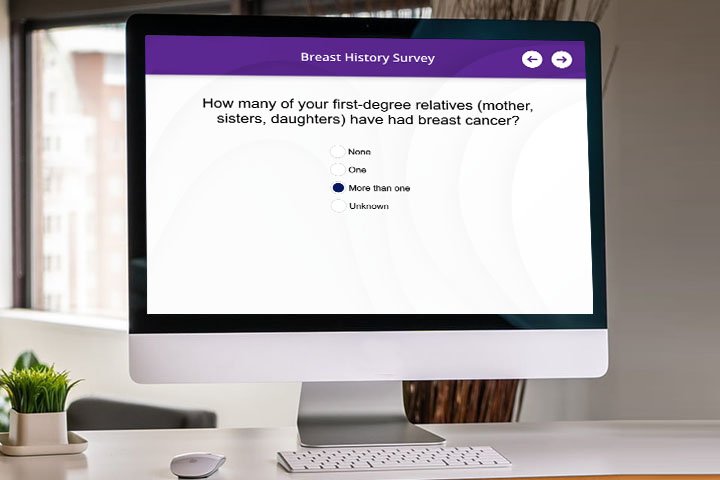
A Mammography Information System (MIS), which can also be referred to as a Mammography Reporting System, is a dedicated sub-specialty software solution that allows breast imaging centers to track and manage all patient data from one central platform.
An MIS offers far greater efficiencies than standard EHR-based mammography tracking modules. If a facility doesn’t have a dedicated MIS, staff are likely tracking patients and statistics manually via spreadsheets.
In the following, we take a look at common reasons breast centers explore using an MIS; common reasons for delay; and steps you can take to help determine whether your breast center would benefit from using one.
Common Reasons Centers Explore Using an MIS
Breast centers and radiology groups can experience many benefits from using an MIS, including optimizing the patient experience. The following are common reasons providers decide to explore a dedicated Mammography Tracking and Reporting System.
MQSA Compliance
The annual MQSA inspection requires intense preparation from breast centers, but an MIS can greatly reduce the stress involved. When the inspectors need data, the MIS makes it readily available in a format that’s easy to understand.
Patient Letters
One MQSA requirement is that patients be notified of their results within 30 days. An MIS can manage all patient notification letters, which include the patient’s breast density. Reminder letters for annual mammograms, or any follow-up interval, are also part of the system.
Patient Tracking Software
An MIS effectively tracks patients in a variety of ways. Even better, an MIS tracks at a lesion level, not a study level. While study-level tracking is common, this method fails to capture the needs of patients who present with multiple lesions or findings from a single study. An MIS is built to ensure no patient slips through the cracks and provides tools to increase patient return rate.
Breast Cancer Risk Assessment Tool
High-risk breast screening has quickly become the standard of care. There are online calculators and stand-alone risk assessment software systems on the market, but the most robust MIS platforms are fully integrated with multiple risk model options, making it easy to screen your entire patient population and flag high risk patients. An MIS automates the process of running risk scores as well as other pieces of the workflow that are essential in setting up and maintaining a high-risk screening program.
Radiologist Structured Reporting
An MIS includes an option for radiologists to create structured results commonly referred to as “point and click” reporting. Radiology reporting Software in an MIS offers the advantage of consistent and uniform results as well as a reduction in liability since it helps to ensure key elements aren’t missed and reduces the chance for errors. Additionally, the workflow integration enabled by structured reporting supports pre-population of patient information as well as automation of the patient’s letter and follow-up protocol. If structured reporting isn’t desired, most MIS systems provide integration with third-party dictation systems.
Workflow Efficiencies
An MIS can add automation to many different areas of a breast imaging center’s workflow and potentially replace manual processes that reduce efficiency and productivity.
Common Reasons Centers Delay MIS Implementation
Let’s take a look at some common reasons businesses delay implementing an MIS, and why these scenarios may actually represent the perfect time to move forward.
“Our volume is low”
An MIS can help any size facility meet patient care, reporting, and MQSA-compliance needs. In fact, due to the manual processes often in use, smaller facilities may be at greater risk of overlooking critical details that could lead to concerns about patient care and liability.
“Our process works”
Although an existing process may seem to work, it’s critical to keep up with the competition. In the ever-changing landscape of healthcare, every facility can benefit from the new, cutting-edge technologies that are integrated into an MIS solution.
“We already have a mammo module with our EHR system”
Although some EHR modules offer basic functionalities to support breast centers, they’re typically quite limited and still require manual processes. In contrast, a dedicated MIS provides sub-specialty software dedicated to meeting unique facility needs to optimize patient care and workflow efficiencies.
Determining Whether Your Center Needs an MIS
If you’re not sure whether your breast center needs an MIS, the following three steps can help guide your research and decision-making journey.
Step 1: Assess your breast imaging workflow.
Answering the following questions about your current workflow can help identify areas that might need to be improved.
- What is your current process for collecting patient history?
- How do the radiologists view the patient’s history?
- How are risk assessment scores being calculated?
- How do your radiologists create their finding reports?
- What is your current process for notifying a patient of their results?
- How long does it take a patient to complete their exam from the time they walk in the door to when they leave?
- What does your technologist workflow look like?
- What is your process for preparing for an MQSA inspection and providing data for meeting accreditation requirements?
Step 2: Define goals and planning needs.
In order to properly prepare, it’s important to include all stakeholders in the discussion to ensure each department’s needs are taken into consideration. The following questions can help inform both goals and the planning process:
- Who would use the MIS?
- Who would take ownership for ensuring training and oversight?
- What are some short-term goals that an MIS will help you achieve?
- What are some long-term goals that an MIS will help you achieve?
Step 3: Evaluate vendors.
There are a whole host of issues to consider when evaluating MIS vendors. For instance, why isn’t a radiology information system (RIS) or electronic health record (EHR) adequate to meet mammography needs? And what types of things should be covered during vendor demonstrations?
In our next post, “What to Ask Vendors When Evaluating Mammography Reporting Systems,” we’ll cover these topics and more. Come back and check it out.












![monitoring breast density shutterstock_1299510538-[Converted]](https://magview.com/wp-content/uploads/2023/05/shutterstock_1299510538-Converted.jpg)