Many breast imaging centers are putting more focus on their high-risk programs. Some larger facilities have already opened specialty high-risk screening facilities to service these patients.
Although there isn’t a cookie-cutter solution for all facilities, there are certain common elements found in successful high-risk programs. This article will explore some of the general requirements and best practices in place at several facilities.
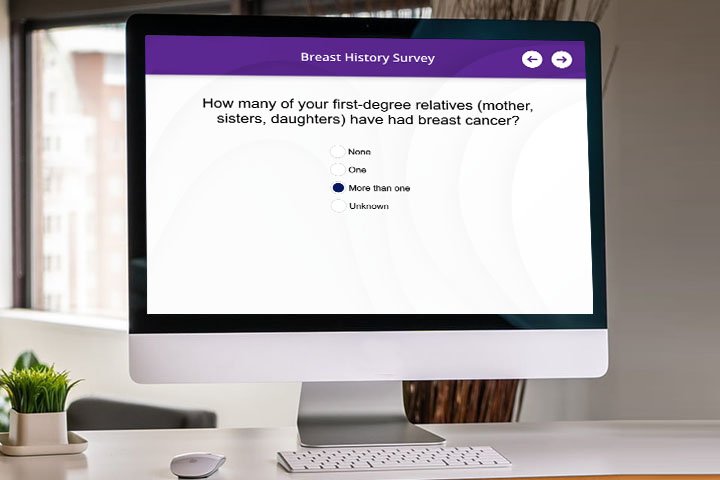
Identification
The first step in creating a high-risk program is identifying which patients qualify as high-risk. There are several risk models available to identify high-risk patients. The NCCN guidelines recommend a high-risk screening protocol for patients who have a lifetime risk of more than 20% as defined by risk models that are largely dependent on family history, including Tyrer-Cuzick, BRCAPRO, and Claus.
Risk Models
The most comprehensive risk model is Tyrer-Cuzick, as it includes more predictive information about the patient’s family. For this reason, it is widely considered the most accurate of the available risk models. In some cases, other risk models are favored because the information gathering requirements are lower. The NCI model predicts the patient’s lifetime risk based on relatively few components of patient history.
Some programs utilize multiple models, as it is possible for a patient to be calculated as high-risk in one model but not another. The benefit of a multi-model approach is two-fold. First, you can identify high-risk patients that fit more than one profile. Second, you can screen patients with faster, less data-intensive models before investing the time in a full family pedigree work up.
Integration
Your high-risk program should be designed to have a minimal impact on your existing workflow. It should minimize additional time spent by patients and technologists, and facilitate your radiologist reading workflow.
Look for integrated risk models that can save your users from having to enter history information into a website or online calculator for every patient. They should be part of the MIS program or accessed behind the scenes in a way that saves everyone time. History data should be retained from year to year so that patients can simply update their history captured at the time of their last screening exam.
High-Risk Tracking
Once you have identified high-risk patients from your screening population, you should track them by using reports or online tools to be sure they are enrolled and participate in your high-risk program. Having the right MIS in place is mission-critical, as you will rely on your system to track their enrollment, education, genetic testing, genetic counseling, and future high-risk screening.
Communication
Once a high-risk patient has been identified, you should consider several ways that can be used individually, or in combination to notify and educate patients about their options.
Referring Provider
Part of the high-risk workflow includes informing the referring physician of their patient’s high-risk status. This allows the physician to start a dialogue with the patient, reinforce their options and provide education. Naturally, a patient might have some anxiety when hearing the term ‘high-risk,’ so it is important for their provider to have all of the necessary information.
Your integrated solution should also have the ability to share a risk score and risk factors in the finding report itself. The more information the provider has to work with, the better informed they will be, and the better informed their patients will be, too.
You may also consider secondary letters to referring physicians, which include lists of their patients which have recently been identified as high-risk. This can be a useful tool for providers and helps ensure they don’t lose track of their high-risk patients.
Patient Notification
Most sites want to keep their patients well informed, and typically include some note about their risk status. This can be as simple as an extra paragraph in the lay result notification letter. It could also be a separate, more complete custom notification specifically sent to your high-risk patient population.
The language can be customized to include specific recommendations about genetic counseling, and offering high-risk screening upon their next visit. It can also include educational material that informs patients about what it means to be high-risk, and what they should do next.
Follow-up
Having notified your patients and their providers, you want to follow up to guide them through the next steps of the program. How do sites proceed from this stage?
Some sites take a hands-on approach to navigating their patients through the continuum of care. This would include phone call reminders and special touchpoints for patients based on their stage in the high-risk program.
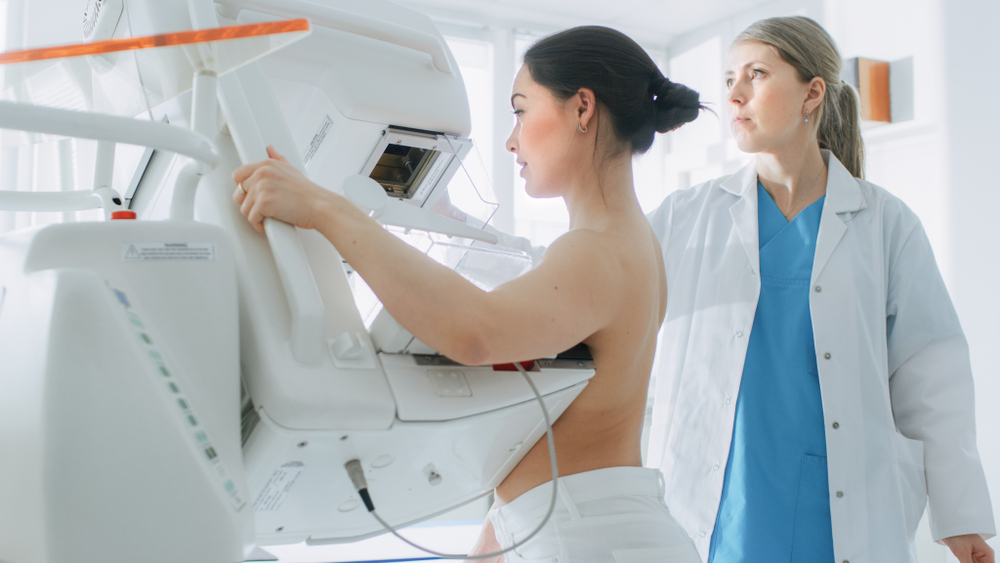
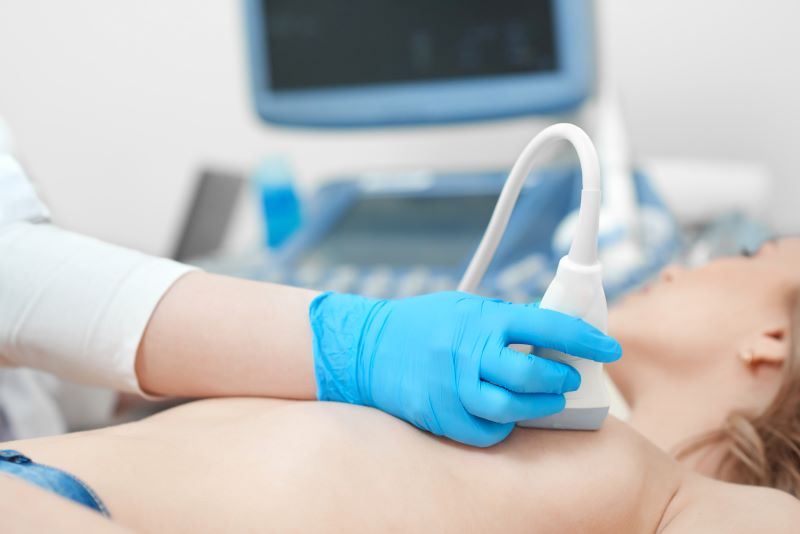
High-Risk Screening
Most sites implement NCCN recommendations, which call for an annual mammogram and a clinical breast exam every 6-12 months, along with an annual breast MRI beginning at age 30. The mammogram and MRI are often staggered so that the patient receives imaging every six months.
Based on high-risk recommendations, any recall letters you send to patients should be configured to call back patients for the appropriate procedures based on your imaging protocol.
Analytics
As a part of tracking your high-risk patients, you should also follow metrics about your high-risk program. You should understand what percent of your patient population is high-risk, and what percent of your high-risk patients are enrolled in your high-risk program. You should also generate quality assurance and outcomes data for your high-risk program and compare it to your non-high-risk program. Being able to track your cancer detection rate, minimal cancer, node-negative cancer and stage 0/I cancer for your high-risk patients can help you measure the success of the program.
MagView offers a specialized toolset for your high-risk program based on the goals and best practices outlined in this article. For more information on how MagView can help you with your high-risk program, please contact your MagView Account Manager today.













![monitoring breast density shutterstock_1299510538-[Converted]](https://magview.com/wp-content/uploads/2023/05/shutterstock_1299510538-Converted.jpg)